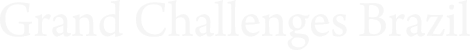Bacteria may indicate risk of premature birth and lead to the development of a new diagnostic test for global use
Antônio Fernandes Moron
Humanity is able to predict storms and asteroids on a collision course with Earth. However, we are still unable to accurately assess when a pregnant woman may have a spontaneous premature delivery, that is, before 37 weeks of gestation. There are currently only two ways to assess this risk: if a woman has had a premature baby before or if a transvaginal ultrasound shows that her cervix is shorter than normal, at under 25 millimeters – in a pregnancy, the cervix functions as a “gate” that separates the baby from the external environment. However, these two methods are only capable of estimating around 40 percent of spontaneous births ahead of time, which today account for two-thirds of premature births in Brazil and 35 percent of the 3.1 million newborn deaths in the world. In places with limited resources and without available ultrasound technology, this predictability is even lower. “Measuring these risks accurately can help us to prolong pregnancy and avoid hospitalizations and deaths of babies,” says obstetrician Antonio Fernandes Moron, Professor at the School of Public Health of the University of São Paulo (USP), postdoctoral fellow in Fetal Medicine at the University of Wisconsin Medical School and professor at the Department of Obstetrics at the Federal University of São Paulo (Unifesp).
In addition to these two factors, research has found that imbalances in the bacteria that normally inhabit the vaginal flora, the microbiome, can also trigger preterm births. In general, those of the Lactobacillus type, common in this area, produce a substance called lactic acid, which makes the environment more acidic and protects the vagina and cervix against the invasion of species that cause infections, such as Gardnerella vaginalis and others. When infections occur, they modify the structure of the cervix and make it softer. This can lead to cervical shortening, which makes women more prone to a premature birth.
The study by Moron’s team aimed to identify whether microorganisms, substances and compounds in the vaginal microbiome, could accurately detect a shortening of the cervix and, therefore, a greater risk of premature birth. “Our goal was to assess whether it was possible to add a third prediction factor to the two that already exist,” says Steven Sol Witkin, professor Emeritus in the Department of Obstetrics and Gynecology at Weill Cornell Medicine, a specialist in reproduction immunologist, and Moron’s research partner. The team collected two vaginal samples from 568 women between 18 and 24 weeks of gestation in hospitals in three Brazilian cities: São Paulo, Jundiaí, and Fortaleza. The length of the cervix was assessed through transvaginal ultrasound. The researchers also analyzed the composition of the vaginal microbiome. Among the 40 species found, three bacteria were the most common: Gardnerella vaginalis, Lactobacillus inners and Lactobacillus crispatus. The latter is largely responsible for increasing the levels of D-lactic acid, an important substrate for maintaining a healthy cervix. The study showed that the combination of low levels of D-lactic acid and high concentration of an inflammation marker, TIMP-1 (tissue inhibitor of metalloproteinase 1), in vaginal secretions represents a reliable indicator that L. crispatus has ceased to predominate in the flora and there is a greater risk of cervical shortening and spontaneous premature delivery. When combined with transvaginal ultrasound, the test was able to identify 71 percent of births before 37 weeks in the sample evaluated, as compared to only 31 percent predicted by the two conventional methods (history and cervical measurement).
The microbiome analysis proved reliable even in the absence of ultrasound, allowing researchers to track around 60% of cases of preterm childbirth. “This demonstrates that the method can be a simple and cost-effective way to assess the prevalence of L. crispatus or other microorganisms and the length of the cervix during pregnancy, without requiring expensive and sophisticated resources such as genetic sequencing,” says Moron. “The results can generate a new test to identify risks of prematurity and establish new protocols.”
The researchers also evaluated 107 of 600 vaginal samples and found, for the first time, that some viruses, called bacteriophages, because they infect bacteria, could also influence the length of the cervix. The team is looking for funding for a new study that would test the method’s effectiveness in the first trimester of pregnancy and the feasibility of turning it into a diagnostic. “Our idea is to create something simple and affordable to use, similar to a pregnancy test,” says Moron. “For the first time in the literature, we also want to assess the influence of viruses on the length of the cervix.”