The study that evaluated magnesium, but found that quality prenatal care is what can decrease premature births
João Guilherme Bezerra Alves
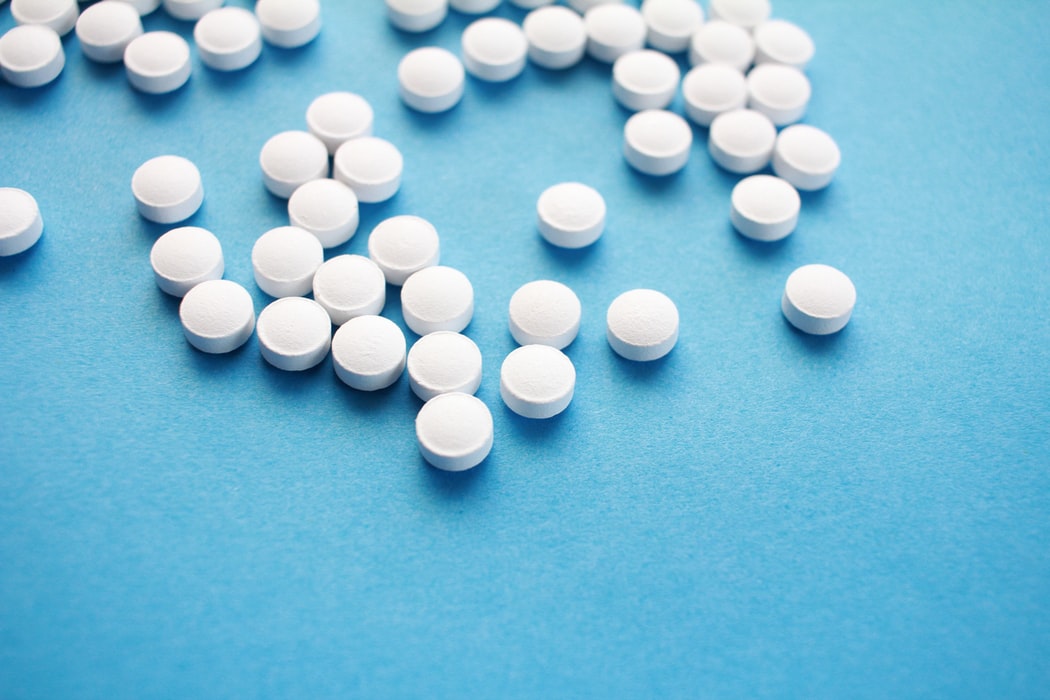
Because it is indispensable in several body processes, magnesium is among the four most important mineral salts for human health. During pregnancy, magnesium deficiency can cause complications that lead to premature birth, such as pre-eclampsia, sudden increase in blood pressure, and other vascular problems in the placenta, such as detachment. The objective of a study by pediatrician and researcher João Guilherme Bezerra Alves, Director of Education and Coordinator of the Graduate Program at the Professor Fernando Figueira Institute of Integral Medicine (IMIP), in Recife (Pernambuco state), was to assess whether supplementing magnesium in the diet of pregnant women could reduce these risks.
The study looked at whether maternal oral supplementation of magnesium citrate tablets, administered before the twentieth week of pregnancy until the end of pregnancy, could decrease the occurrence of premature births for spontaneous or medically induced reasons, such as high blood pressure and other complications. Cheap and easy to manufacture, the pills were produced at the IMIP pharmacy. If they prove effective, they could be a low-cost option to reduce prematurity, especially in countries with few resources.
The team recruited 911 pregnant women in prenatal care from three hospitals in Pernambuco. Of this total, 449 received the magnesium citrate tablets and 462 received a placebo. They were randomly divided between the two groups and only one member of the team knew what was being administered to each of them, a so-called double-blind, randomized trial, considered one of the most reliable methods in science.
Around the twentieth week of gestation, all pregnant women began taking the pills (with or without magnesium) and were followed up until the end of the pregnancy. They had similar social, demographic, behavioral, income – between 1.6 and 2 minimum wages – and biological characteristics. Due to changes in prenatal care, the Zika virus epidemic (in 2015) and adverse reactions of the pills reported in both groups, 82 women dropped out of the study. “Despite, the sample had sufficient statistical power,” guarantees Alves. The study found no differences among pregnant women who took magnesium citrate and pregnant women who took the placebo in the incidence of premature births, the number of stillborn babies, or the number of babies who were small for gestational age (SGA). The mineral also had no effect on the occurrence of pre-eclampsia and placental abruption, even after adjusting for differences in socioeconomic, demographic, and environmental risk factors. “It was important to scientifically demonstrate that magnesium, in isolation, has no protective or preventive effect for premature birth,” says Alves. The mortality of newborn babies was much lower among mothers who took the magnesium pills. “There is a hypothesis that magnesium may confer neuroprotection to the newborn,” says the researcher. “However, it will be necessary to investigate this finding further in order to understand it and prove the causal relationship.”
At the beginning of the study, 31 percent of pregnant women had magnesium deficiency and this rate declined as the pregnancy progressed. The frequency of premature birth among the 911 participating pregnant women was 7 percent, much lower than the Brazilian average of 11.5 percent, according to the latest survey by the National School of Public Health (ENSP / Fiocruz) in 2016. According to the researchers, one explanation may be the greater care available to and reception of the pregnant women who agreed to join the study. Participants in the study had guaranteed a priority prenatal service, in addition to permanent contact with the team. “This demonstrates the importance of quality service for the reduction of premature births,” says the pediatrician.